University of Massachusetts
Worcester, MA
Program Director: Scott Kopec, MD
Type of Program: Pulmonary and Critical Care
Abstract Authors: Rahul N. Sood, MD; Paolo J. Oliveria, MD; Sukary Touray, MD; and Jared Mickleson, MD
RATIONALE
Pulmonary and critical care physicians are often involved in managing critically ill patients with marginal cardio-pulmonary reserve, who require urgent endotracheal intubation (ETI) in the medical intensive care units (ICU). This is often a high risk/ high stakes situation. Advanced airway management competency is a required core skill for pulmonary/ critical care medicine (PCCM) fellows. To effectively evaluate and accomplish this educational goal, it is important to understand fellow attitudes and learning needs in this domain. We will use our programs’ baseline data to help implement a structured airway management curriculum. Currently, at UMass Memorial Medical Center the vast majority of intubations in the ICU are performed by anesthesia residents. A survey of our PCCM fellows conducted last year showed that 88 percent of PCCM fellows had performed fewer than 10 ETIs across all levels of training. This represents a clear deficiency in our curriculum.
METHODS
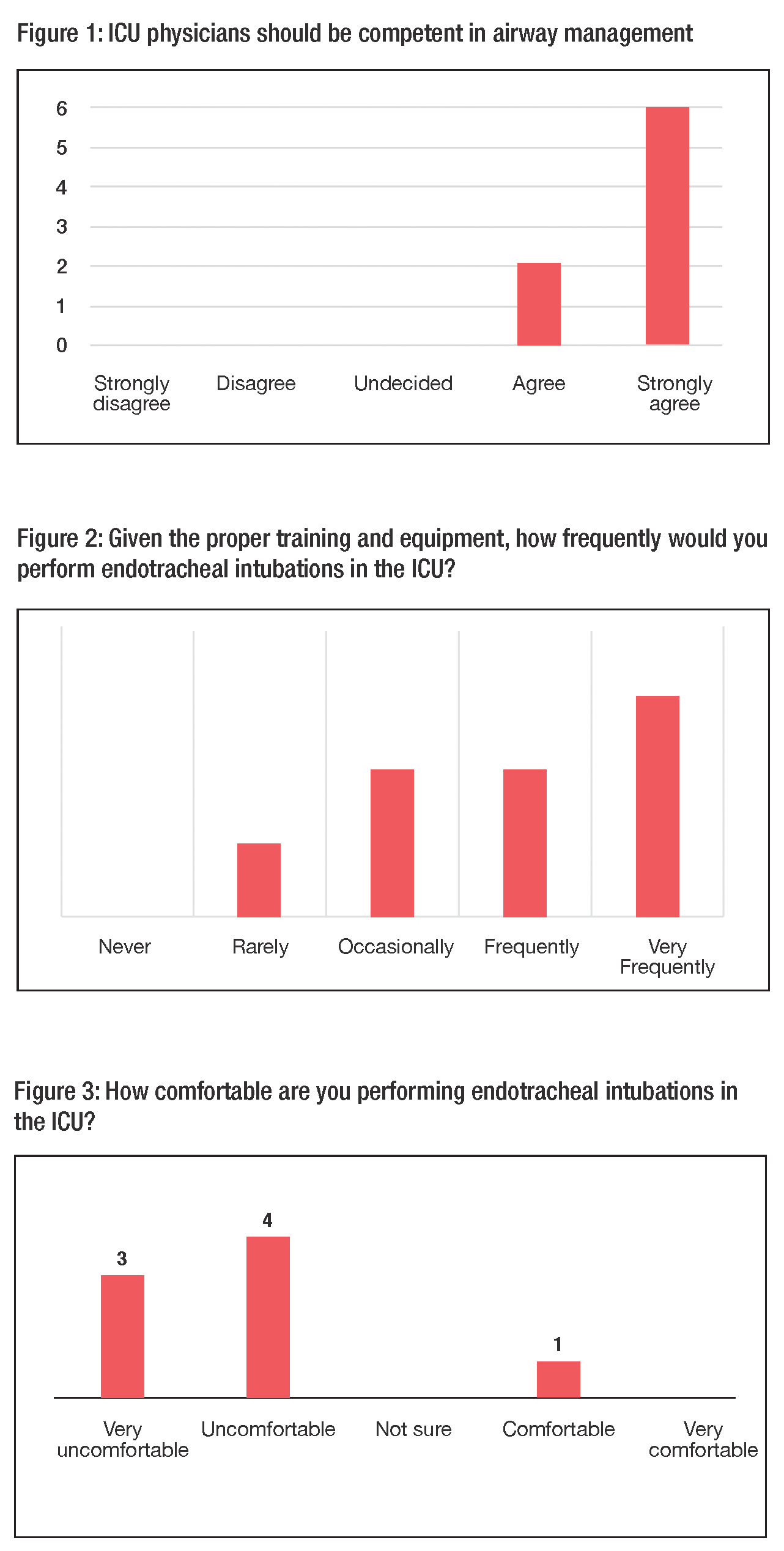
An anonymous 5-question online survey was emailed to all 9 UMass PCCM fellows to assess their learning needs, attitudes, and comfort level surrounding advanced ICU airway management using a 5-point Likert scale.
EVALUATION
A completed survey was returned by 8 out of 9 fellows. Of the respondents, 7 out of 8 felt uncomfortable managing urgent ICU airway-related issues and believed they would benefit from formal training. The survey also, importantly, revealed that our fellows would not feel comfortable managing the airway in critically ill patients after graduating should they seek employment at hospitals where they are relied upon as the primary airway managers. Based on this gap in fellowship education, we plan to implement a multi-domain competency-based curriculum and assessment process to assist fellows in acquiring the confidence, cognitive aptitude, and technical expertise in critical care airway scenarios as part of the curriculum over the next 3 years.
CONCLUSIONS
The majority of PCCM fellows at our institution who recently responded to an anonymous online survey reported that they felt uncomfortable performing urgent ETI in the ICU, would benefit from formal training, and desired to achieve competence in advanced airway management. We aim to implement a novel airway management curriculum consisting of didactics, case-based scenario learning, and hands-on training with senior anesthesia staff to maximize fellows’ comfort level with intensive care intubations that when tracked longitudinally after graduation will translate into the rectification of our current curricular training deficit.