Authors: Dr. Peter Klijn, clinical exercise physiologist
Merem Medical Rehabilitation, department of Pulmonary Rehabilitation
Hilversum, The Netherlands
Exercise training is a cornerstone of pulmonary rehabilitation (PR) with the combination of aerobic endurance training and strength training as major parts. [1] The prevailing PR exercise paradigm could be characterized as a multimodal, continuous program, i.e. similar whole-body endurance exercises (walking and cycling) and number of resistance training (RT) exercises with constant sets and repetitions for the duration of the program. However, the use of such a concurrent exercise paradigm, especially performed in the same session (i.e. cycling, walking and strength training), could hamper physiological adaptations. [2-11]
Improving different physical fitness characteristics (e.g. muscular strength, anaerobic endurance, power, speed, muscular endurance, aerobic endurance) within a timeframe is common practice in the athletic population. It is therefore crucial to properly organize the training plan. Athletes use exercise periodization to achieve peak performance at a predetermined point in time. [8] There is, however, a major difference in time frames of athletic training and PR. An in-depth discussion of athletic periodization theory, [8, 12, 13] however, is beyond the scope of this quarterly bite.
Periodization is characterized by a division in interrelated periods, i.e. smaller, distinct and more easy manageable phases each with specific goals and characteristics. [14-16] Each phase contains microcycles (typically one week). The objectives of these phases and cycles all contribute to the overall training plan. [8] The microcycle consists of several training sessions (typically 3/week during PR). The training session is the smallest functional unit and determines the characteristic and focus of the microcycle. [8] Figure 1 illustrates an example of a training plan during PR divided into phases and cycles.
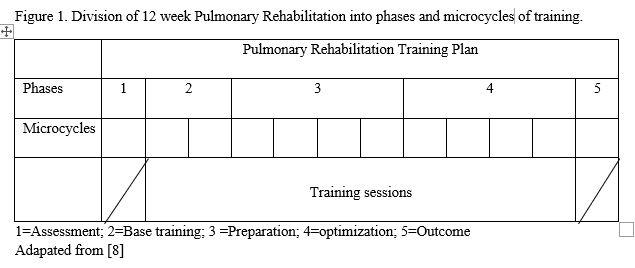

Moreover, the concept of periodization involves the process of systematic planning of short- and long-term training by manipulating acute training variables to optimize the fundamental exercise principle of overload, i.e. gradual increase in the stimulus placed on the body to stimulate continual adaptation.
Variation, i.e. appropriate sequencing and integration of different acute training variables, is a key tenet of periodization. By incorporating variation of training variables the body is regularly challenged to restore the disruption of (muscle) homeostasis, thereby preventing stagnation and ultimately, optimize adaptations (i.e. supercompensation). [17, 18]
The planning process (i.e. training phases) aims to develop specific physical fitness characteristics (e.g. muscular strength, anaerobic endurance, power, muscular endurance, aerobic endurance) that contribute to the specific goal. The training program typically starts with a base training phase. This is a physiological and psychological adaptation phase characterized by a low load:
- to familiarize patients with the exercises
- to become accustomed to the combination of exercises
- to improve neuromuscular function
- to develop or improve training technique (e.g. breathing technique, speed of muscle action, adequate time-under-tension, duration of concentric and eccentric phases)
- to teach patients the theory and methodology of goal specific training
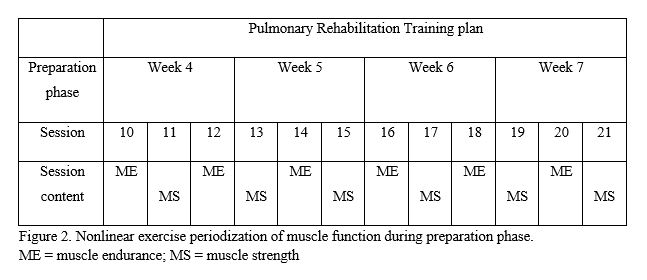
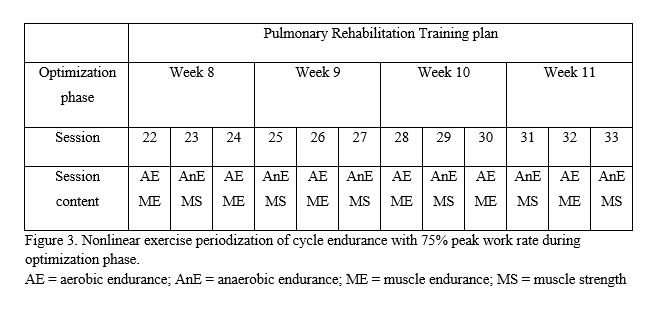
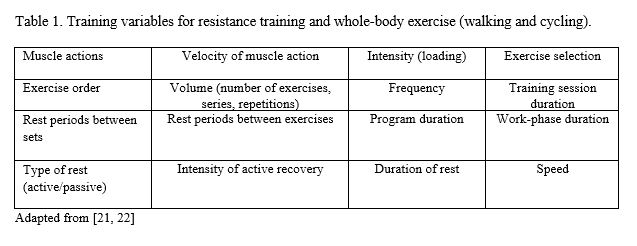
In the preparation phase patients are prepared for more intense exercise. The use and appropriate structuring of selected acute training variables (i.e. programming) elicits the required adaptations (e.g. musculoskeletal, neuromuscular, metabolic). [19] An example preplanned 4-week preparation phase is shown in Figure 2. During the optimization phase protocols are used to induce goal specific adaptations. Figure 3 shows an example of a preplanned 4-week optimization phase. The duration of each training phase is, however, not fixed, but depends on the time needed by the individual patient for adequate preparedness or improvement of the physical fitness attribute(s). Appropriate planning and programming prevents overtraining, modulate accumulative fatigue and attain an optimal training effect. [20, 21] As shown in table 1 there is a multitude of possible combinations between program variables and hence, many possible periodized programs. [18]
As stated above, periodization is a fundamental strategy to organize exercise training in athletic populations. [21, 23] However, during the last decade exercise periodization has also received considerable interest as a defining principle in health-indices, the rehabilitation setting and the old. [24-33] Although there are different types of periodization, this quarterly bite will focus on non-linear periodization. [21]
Nonlinear or undulating periodization is a type of periodization characterized by frequent manipulation of training variables and often dramatic alterations in the exercise intensity, repetition volume and number of exercises. [20] The undulating model makes these changes daily, weekly, or biweekly. Recently, nonlinear periodized exercise training (NLPE) with a daily undulating model was compared with traditional endurance and progressive resistance training (EPR) in patients with severe to very severe COPD. [20] Superior statistical significant and clinical relevant larger improvement in endurance cycling and all domains of the Chronic Respiratory Questionnaire, was achieved with NLPE compared to EPR. EPR was a traditional, multimodal continuous program. In this regard, it is important to emphasize again that concurrent and continuous, high-intensity linear loads, absent of variation may increase the risk of maladaptation. [8-10, 34]
The development of an individual training program during PR requires a realistic, achievable goal and goal specific exercise assessment (i.e. consistency between training and testing). Moreover, it is paramount to perform a needs analysis of the required physical activity (e.g. walking, stair climbing, carrying groceries, cycling). The needs analysis includes a physiological and biomechanical analysis, and an analysis of individual deficiencies. [16, 35]
-physiological analysis: to determine, among others, which energy sources are used and what are the determining muscle attributes (e.g. strength, power, endurance) distinctive to the physiological profile of the physical activity.
- biomechanical analysis: involved joints, joint range of motion, muscle groups and types of movement to choose activity-specific training.
The resultant of the performance needs analysis therefore, dictates the building blocks of individual training programs. The needs analysis and, physiological and biomechanical building blocks of the recent NLPE intervention is shown in table 2.
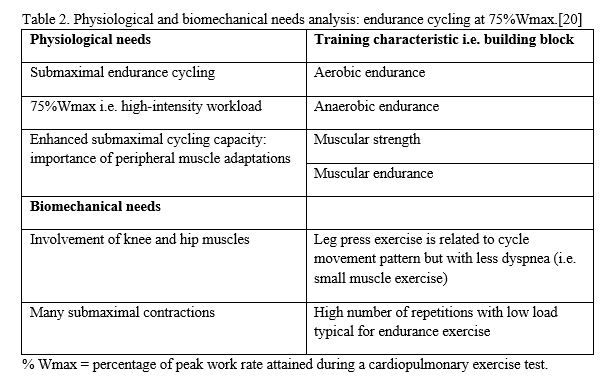
A building block (e.g. aerobic endurance) consists of several protocols composed of different combinations of the training variables (e.g. duration of work phase, intensity, duration of rest phase, number of series). The focus of the aerobic endurance training session can be achieved with different acute training variables (Table 1) determined by the needs of a patient pertaining to cycling with 75% Wmax
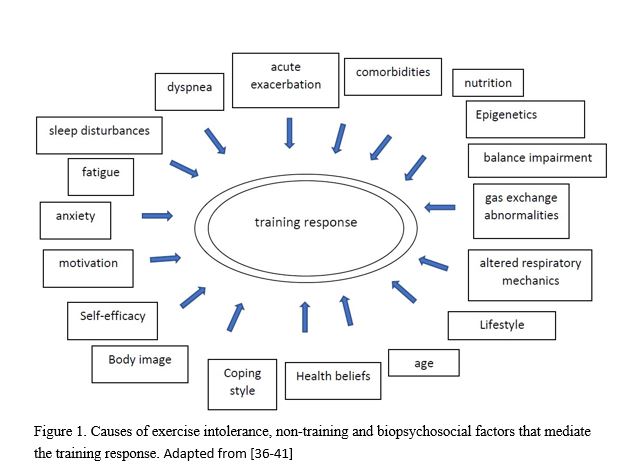
The analysis of deficiencies provides information on the individual causes of exercise intolerance and biopsychosocial factors that mediate the training response, and should therefore be addressed in the individual training plan. As can be observed in Figure 1, there is myriad of factors that could influence the response to exercise training. Furthermore, these factors are prevalent in many combinations. Based on the needs analysis (i.e. physiological and biomechanical building blocks) a global preplanned individual training plan (i.e. training phases) should be developed. The preplanned programming (i.e. exercise protocols) is determined by the analysis of exercise intolerance and non-training factors. In this respect it is important to emphasize that physical activity during daily life has implications for the recovery-adaptation relationship, since every physical activity is a challenge to homeostasis. Clearly, outpatient PR is more likely to be influenced by non-training factors.
Next to the needs analysis, the actual programming is determined by emerging information from the training sessions (i.e. monitoring). Monitoring is an imperative element in exercise periodization that unveils how patients respond to the training, thereby enhancing individualization and recovery. [42] The monitoring process actually starts before the training session with an assessment of prevalent symptoms: global fatigue (i.e. highly prevailing and disabling symptom in COPD), [43] level of dyspnea (i.e. day-to-day variability) and sympathetic stress (i.e. heart rate and percutaneous oxygen saturation [SpO2]). [20] During a training session emerging symptoms (exercise-induced dyspnea and muscle fatigue, sense of effort) should be assessed and after the training session the transient training stress is evaluated (i.e. residual fatigue, dyspnea, heart rate and SpO2). [20] These detailed monitoring records are necessary to establish individual patterns for further planning and programming, and eliciting desired goal specific training effects. [15] In this respect it is important to consider the high level of subjectivity that is characteristic of bodily symptoms (e.g. dyspnea, fatigue, exertion or heaviness, pain). [44-47] Clearly, the preplanned format determines the basics of the program. Exercise protocols, however, are adapted based on the emerging information from the training sessions.
A multitude of factors play a role in the variable adaptation to exercise training in patients with COPD. Clearly, there is a need for personalized exercise training based upon a comprehensive assessment and systematic research on the individual exercise response to establish the interfering factors of exercise adaptation. Nonlinear exercise periodization might provide a template for the organization of exercise training in the heterogenous COPD population.
References
- Spruit MA, Singh SJ, Garvey C, Zuwallack R, Nici L, Rochester C, Hill K, Holland AE, Lareau SC, Man WD et al: An official American Thoracic Society/European Respiratory Society statement: key concepts and advances in pulmonary rehabilitation. Am J Respir Crit Care Med 2013, 188(8):e13-e64.
- Casaburi R: Getting serious about strength training. J Cardiopulm Rehabil 2006, 26(5):338-340.
- Mador MJ, Bozkanat E, Kufel TJ: Quadriceps fatigue after cycle exercise in patients with COPD compared with healthy control subjects. Chest 2003, 123(4):1104-1111.
- Mador MJ, Deniz O, Aggarwal A, Kufel TJ: Quadriceps fatigability after single muscle exercise in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2003, 168(1):102-108.
- Mador MJ, Kufel TJ, Pineda LA, Steinwald A, Aggarwal A, Upadhyay AM, Khan MA: Effect of pulmonary rehabilitation on quadriceps fatiguability during exercise. Am J Respir Crit Care Med 2001, 163(4):930-935.
- Saey D, Debigare R, Leblanc P, Mador MJ, Cote CH, Jobin J, Maltais F: Contractile leg fatigue after cycle exercise: a factor limiting exercise in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2003, 168(4):425-430.
- Saey D, Michaud A, Couillard A, Cote CH, Mador MJ, Leblanc P, Jobin J, Maltais F: Contractile fatigue, muscle morphometry, and blood lactate in chronic obstructive pulmonary disease. Am J Respir Crit Care Med 2005, 171(10):1109-1115.
- Bompa TO, Haff GG: Periodization: Theory and methodology of training., 5th edn. Champaign (IL): Human Kinetics; 2009.
- Hawley JA: Molecular responses to strength and endurance training: are they incompatible? Appl Physiol Nutr Metab 2009, 34(3):355-361.
- Hickson RC: Interference of strength development by simultaneously training for strength and endurance. Eur J Appl Physiol Occup Physiol 1980, 45(2-3):255-263.
- Kraemer WJ, Patton JF, Gordon SE, Harman EA, Deschenes MR, Reynolds K, Newton RU, Triplett NT, Dziados JE: Compatibility of high-intensity strength and endurance training on hormonal and skeletal muscle adaptations. Journal of applied physiology (Bethesda, Md : 1985) 1995, 78(3):976-989.
- Issurin VB: New horizons for the methodology and physiology of training periodization. Sports Med 2010, 40(3):189-206.
- Wathen D, Beachle TR, Earle RW: Periodization. In: Essentials of strength training and conditioning: National Strength and Conditioning Association. Third edn. Edited by Baechle Tr, Earle RW. Omaha, Nebraska: Human Kinetics; 2008: 505-522.
- DeWeese BH, Horsby G, Stone M, Stone MH: The training process: Planning for strength–power training in track and field. Part 2: Practical and applied aspects. J Sport Health Sci 2015, 4(4):318-324.
- Hoover DL, VanWye WR, Judge LW: Periodization and physical therapy: Bridging the gap between training and rehabilitation. Physical therapy in sport : official journal of the Association of Chartered Physiotherapists in Sports Medicine 2016, 18:1-20.
- Turner A: The science and practice of periodization: a brief review. Strength and Conditioning journal 2011, 33(1):34-46.
- Naclerio F, Moody J, Chapman M: Applied Periodization: A Methodological Approach. J Hum Sport Exerc 2013, 8(2):350-366.
- Rhea MR, Ball SD, Phillips WT, Burkett LN: A comparison of linear and daily undulating periodized programs with equated volume and intensity for strength. J Strength Cond Res 2002, 16(2):250-255.
- Cunanan AJ, DeWeese BH, Wagle JP, Carroll KM, Sausaman R, Hornsby WG, 3rd, Haff GG, Triplett NT, Pierce KC, Stone MH: The General Adaptation Syndrome: A Foundation for the Concept of Periodization. Sports Med 2018, 48(4):787-797.
- Klijn P, van Keimpema A, Legemaat M, Gosselink R, van Stel H: Nonlinear exercise training in advanced chronic obstructive pulmonary disease is superior to traditional exercise training. A randomized trial. Am J Respir Crit Care Med 2013, 188(2):193-200.
- American College of Sports Medicine Medicine: American College of Sports Medicine position stand. Progression models in resistance training for healthy adults. Med Sci Sports Exerc 2009, 41(3):687-708.
- Slade SC, Keating JL: Exercise prescription: a case for standardised reporting. British journal of sports medicine 2012, 46(16):1110-1113.
- PB. L: Training for intense exercise performance: high-intensity or high-volume training? Scand J Med Sci Sports 2010, 20 Suppl 2:1-10.
- Blanchard S, Glasgow P: A theoretical model to describe progressions and regressions for exercise rehabilitation. Physical therapy in sport : official journal of the Association of Chartered Physiotherapists in Sports Medicine 2014, 15(3):131-135.
- Botero JP, Shiguemoto GE, Prestes J, Marin CT, Do Prado WL, Pontes CS, Guerra RL, Ferreia FC, Baldissera V, Perez SE: Effects of long-term periodized resistance training on body composition, leptin, resistin and muscle strength in elderly post-menopausal women. The Journal of sports medicine and physical fitness 2013, 53(3):289-294.
- Conlon JA, Newton RU, Tufano JJ, Penailillo LE, Banyard HG, Hopper AJ, Ridge AJ, Haff GG: The efficacy of periodised resistance training on neuromuscular adaptation in older adults. European journal of applied physiology 2017, 117(6):1181-1194.
- de Freitas MC, de Souza Pereira CG, Batista VC, Rossi FE, Ribeiro AS, Cyrino ES, Cholewa JM, Gobbo LA: Effects of linear versus nonperiodized resistance training on isometric force and skeletal muscle mass adaptations in sarcopenic older adults. Journal of exercise rehabilitation 2019, 15(1):148-154.
- Foschini D, Araujo RC, Bacurau RF, De Piano A, De Almeida SS, Carnier J, Rosa TD, De Mello MT, Tufik S, Damaso AR: Treatment of obese adolescents: the influence of periodization models and ACE genotype. Obesity (Silver Spring, Md) 2010, 18(4):766-772.
- Kiwata JL, Dorff TB, Todd Schroeder E, Salem GJ, Lane CJ, Rice JC, Gross ME, Dieli-Conwright CM: A pilot randomised controlled trial of a periodised resistance training and protein supplementation intervention in prostate cancer survivors on androgen deprivation therapy. BMJ open 2017, 7(7):e016910.
- Pegrum J, Dixit V, Padhiar N, Nugent I: The pathophysiology, diagnosis, and management of foot stress fractures. The Physician and sportsmedicine 2014, 42(4):87-99.
- Reiman MP, Lorenz DS: Integration of strength and conditioning principles into a rehabilitation program. Int J Sports Phys Ther 2011, 6(3):241-253.
- Zanetti HR, Cruz LG, Lourenco CL, Neves Fde F, Silva-Vergara ML, Mendes EL: Non-linear resistance training reduces inflammatory biomarkers in persons living with HIV: A randomized controlled trial. European journal of sport science 2016, 16(8):1232-1239.
- Zanetti HR, da Cruz LG, Lourenco CL, Ribeiro GC, Ferreira de Jesus Leite MA, Neves FF, Silva-Vergara ML, Mendes EL: Nonlinear Resistance Training Enhances the Lipid Profile and Reduces Inflammation Marker in People Living With HIV: A Randomized Clinical Trial. Journal of physical activity & health 2016, 13(7):765-770.
- Williams TD, Tolusso DV, Fedewa MV, Esco MR: Comparison of Periodized and Non-Periodized Resistance Training on Maximal Strength: A Meta-Analysis. Sports Med 2017, 47(10):2083-2100.
- Fleck SJ, Kraemer WJ: Developing the individualized resistancetraining workout. In: Designing resistance training programs. edn. Edited by Fleck SJ, Kraemer WJ: Human Kinetics; 2005: 151-186.
- Giardino ND, Curtis JL, Andrei AC, Fan VS, Benditt JO, Lyubkin M, Naunheim K, Criner G, Make B, Wise RA et al: Anxiety is associated with diminished exercise performance and quality of life in severe emphysema: a cross-sectional study. Respir Res 2010, 11(1):29.
- Lee AL, Holland AE: Time to adapt exercise training regimens in pulmonary rehabilitation--a review of the literature. International journal of chronic obstructive pulmonary disease 2014, 9:1275-1288.
- Kiely J: Periodization paradigms in the 21st century: evidence-led or tradition-driven? Int J Sports Physiol Perform 2012, 7(3):242-250.
- Lagerwaard B, Nieuwenhuizen AG, de Boer VCJ, Keijer J: In vivo assessment of mitochondrial capacity using NIRS in locomotor muscles of young and elderly males with similar physical activity levels. GeroScience 2020, 42(1):299-310.
- Sharples AP, Polydorou I, Hughes DC, Owens DJ, Hughes TM, Stewart CE: Skeletal muscle cells possess a 'memory' of acute early life TNF-alpha exposure: role of epigenetic adaptation. Biogerontology 2016, 17(3):603-617.
- Thiel A, Sudeck G, Gropper H, Maturana FM, Schubert T, Srismith D, Widmann M, Behrens S, Martus P, Munz B et al: The iReAct study - A biopsychosocial analysis of the individual response to physical activity. Contemporary clinical trials communications 2020, 17:100508.
- DeWeese BH, Gray H, Sams M, Scruggs S, Serrano A: Revising the definition of periodization: merging historical principles with modern concern. Olymp Coach 2013, 24(1):5-19.
- Goertz YMJ, Spruit MA, Van 't Hul AJ, Peters JB, Van Herck M, Nakken N, Djamin RS, Burtin C, Thong MSY, Coors A et al: Fatigue is highly prevalent in patients with COPD and correlates poorly with the degree of airflow limitation. Therapeutic advances in respiratory disease 2019, 13:1753466619878128.
- Coyne JOC, Gregory Haff G, Coutts AJ, Newton RU, Nimphius S: The Current State of Subjective Training Load Monitoring-a Practical Perspective and Call to Action. Sports medicine - open 2018, 4(1):58.
- O'Donnell DE, Ora J, Webb KA, Laveneziana P, Jensen D: Mechanisms of activity-related dyspnea in pulmonary diseases. Respir Physiol Neurobiol 2009, 167(1):116-132.
- Parshall MB, Schwartzstein RM, Adams L, Banzett RB, Manning HL, Bourbeau J, Calverley PM, Gift AG, Harver A, Lareau SC et al: An official American Thoracic Society statement: update on the mechanisms, assessment, and management of dyspnea. Am J Respir Crit Care Med 2012, 185(4):435-452.
- Williams M, Cafarella P, Olds T, Petkov J, Frith P: Affective descriptors of the sensation of breathlessness are more highly associated with severity of impairment than physical descriptors in people with COPD. Chest 2010, 138(2):315-322.



