Henry Ford Hospital
Detroit, MI
Program Director: Geneva Tatem, MD
Program Type: Pulmonary and Critical Care Medicine
Abstract Authors: Rana Awdish MD, Michael Mendez MD, Geneva Tatem MD, Maria Kokas PhD, Kristen Chasteen MD, Dana Buick MD
RATIONALE
Even as more trainees benefit from simulation-based communications training, the struggle to bring the skills to the bedside remains. In an effort to more consistently utilize the communication skills taught during the training in clinical practice, our institution developed three unique adjuncts to the training.
1. Faculty trained in real-time feedback
2. Faculty led pre-session huddle and post-session debrief
3. An integrated smart phone App for real-time recall of skills
EDUCATIONAL STRATEGY
The Caring Conversations Program at Henry Ford was created to bridge this gap in training. The program focuses on communication skills training for complex, often difficult conversations. It allows trainees to practice new skills, and receive real-time feedback prior to taking those skills to the bedside.
The teaching method includes highly skilled facilitators (RA, DB, KC, MM) and specifically trained improvisational actors guiding the learner through progressively more complex learning opportunities. Cases are structured to keep trainees on their ‘learning edge’ and are practiced in a high-impact, yet safe-to- experiment environment; self-discovery is fostered; and in-unit real-time feedback is integrated for each trainee. Each program element is structured to optimize compatibility with clinical and patient needs and trainee behavioral change.
In order to bridge skills to the bedside, faculty members are trained to give real time feedback with gradually increased degrees of autonomy during family meetings. By training faculty in the same method as the trainees, the language around the skills is consistent, as is the communication model. During the family meeting time-out, trainees are asked to self-identify a skill prior to an encounter, and during the post-meeting debrief faculty offer formative feedback and guide the learner to self-identify a stuck-point and a strategy for addressing it in future encounters. A Caring Conversations App was developed to allow the trainees to access the tools in real time prior to the encounter, available on iTunes and GooglePlay.
IMPLEMENTATION
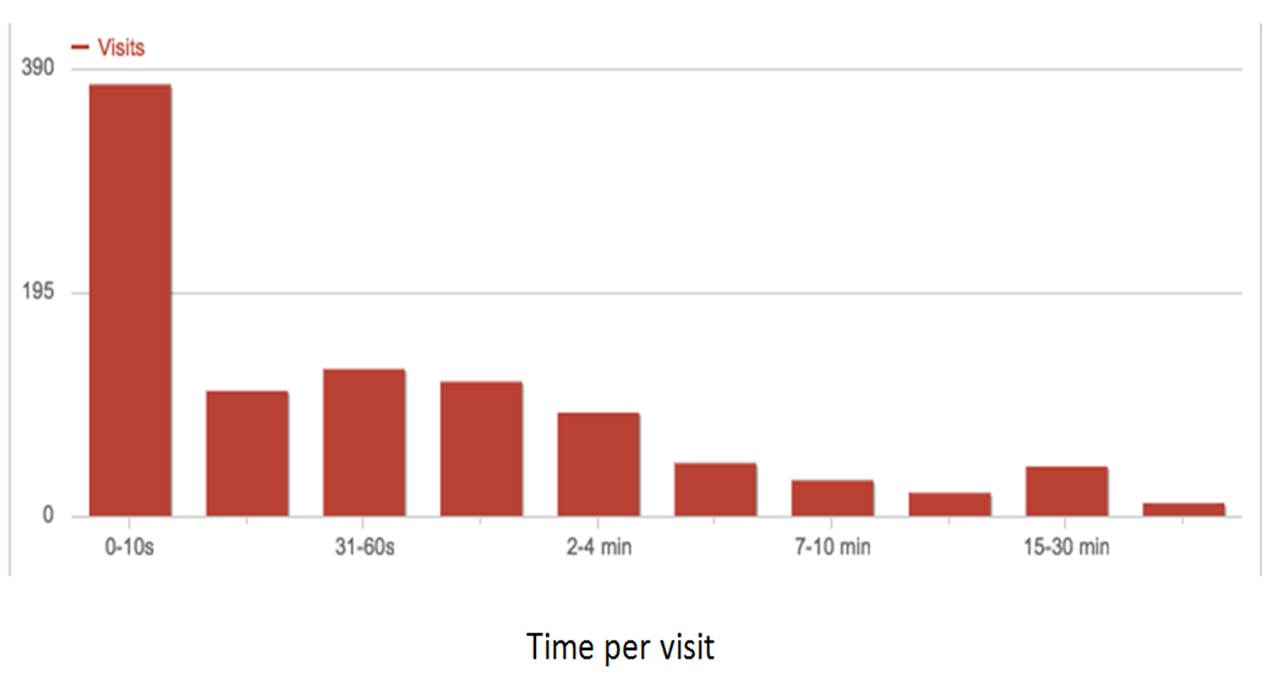
Since 2013, all medical critical care fellows at Henry Ford have participated in 1-3 day workshops where they have an opportunity to practice specific communication skills (Table 1). In addition, all PGY2 Internal Medicine residents participate in three 2.5 hour sessions in which they practice in three areas – 1) Responding to emotion with empathy, 2) Discussing serious news, and 3) Eliciting patient values. Beginning in 2014, critical care faculty began receiving specific training teaching in real time (Table 2) through workshops led by the Caring Conversations faculty. Since 2013, 60 internal medicine residents and 30 critical care fellows have participated in the Communication Skills program. Since 2014, 11 faculty have participated in the Teaching in Real Time program. Figure 1 shows the number of times the Caring Conversations mobile App has been accessed since its inception. Figure 2 illustrates the widespread dissemination of programmatic content via the App. From the small group of US residents who have undergone training, the App has spread organically onto multiple continents. Figure 3 illustrates time per visit on the App ranges from 10 seconds to over 30 minutes, suggesting some are using the content for a quick refresher, while others are reading the content in its entirety.

Figure1. Visits to Caring Conversations App
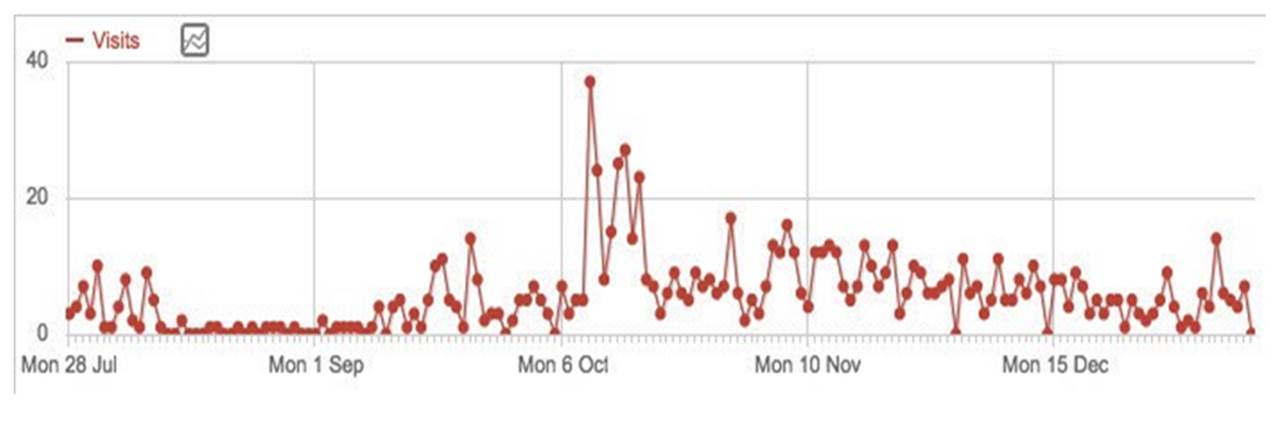
Figure2. Visits to Caring Conversations App by location since July 2014
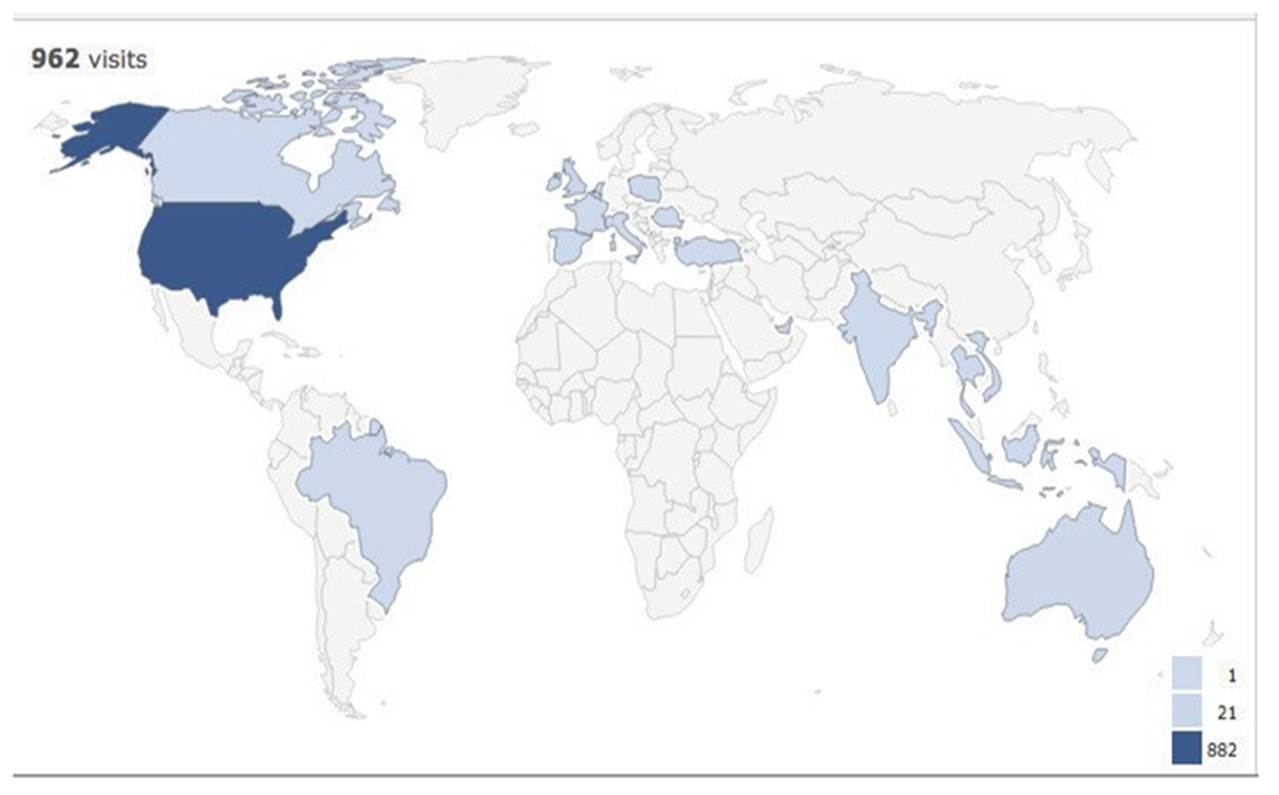
Figure3. Time spent on Caring Conversations App