Mayo Clinic
Rochester, MN
Program Director: Kannan Ramar, MD
Program Type: Pulmonary and Critical Care Medicine
Abstract Authors: Darlene R. Nelson, MD, Travis Wilson, MD, Karen Swanson, MD, Kianoush Kashani, MD, Kannan Ramar, MD
INTRODUCTION
Mentorship is vital to success in any field of medicine. It is recognized as an important influence on career selection, academic advancement and productivity, promotion and satisfaction. Despite this, mentorship is often undervalued in academic medicine and, the development of these vital relationships is challenged by increasing clinical, research and administrative demands. To address these issues, we devised and incorporated an innovative mentorship program for our first year fellows. The program was designed based on results from a comprehensive mentoring survey administered to current faculty, fellows and past fellows. The survey assessed the current state of ‘mentoring’ and identified barriers and characteristics needed to help promote an effective mentoring relationship. We then evaluated the impact after successfully implementing the mentorship program.
METHOD
A baseline survey was conducted among current fellows (n=16) and faculty (n=50), and past fellows (n=19) within the PCCM division to assess the importance of mentorship and identify barriers to successfully implement an effective mentorship program. Surveys were received from 62/85 participants (72.9%). A formalized mentoring program was then initiated for the incoming first year PCCM fellows to help meet the following objectives: goal setting, career planning, address work-life balance, increase the fellows’ academic productivity and career satisfaction during fellowship.
Initially, the fellows’ career interests and plans, goals and objectives with the mentorship, along with their personality characteristics were identified by the program leadership to aid in pairing them with interested faculty. A one hour mentoring workshop was conducted at the beginning of the program for both mentors and mentees. (Table 1) Effectiveness of the program was assessed through quarterly surveys, a validated evaluation form (Berk 2005), semi-structured interviews at the end of one year and review of fellows’ curriculum vitas for publications.
RESULTS
Baseline mentoring surveys identified several themes. First, mentoring was identified as important in medicine (100%) and influenced career choice (60%). Areas of greatest perceived importance were in academic promotion (77%), career planning (80%), and goal achievement (80%). Past fellows expressed a desire to have been matched with a mentor during fellowship (90%) and preferred more help with career planning (56%). Among current fellows, 28% did not identify a mentor and 90% desired more help with career planning. Faculty and fellows differed in the perceived benefit of mentoring related to institutional politics (74% faculty vs. 56% fellows) and work-life balance (85% fellows’ vs 55% faculty), demonstrating how the focus of mentoring relationships may change over time. Several barriers to effective mentorship were identified, including lack of familiarity with faculty interests, not knowing how to initiate a mentoring relationship and time commitment. (Chart 1) These barriers were addressed as we devised and incorporated our mentorship program for the first year fellows.
Mentoring effectiveness was assessed after one year using a previously validated tool (Berk 2005). This scale assesses twelve essential mentoring characteristics and can be used to help evaluate and provide feedback on mentoring. The median score and interquartile range for each item is listed in table 2. Academic productivity over the first year of fellowship increased (18 vs 2 publications, p=0.02) after the initiation of the mentoring program. Semi-structured qualitative interviews demonstrated increased satisfaction by all fellows involved. Statements from involved fellows included “My mentor provided a safe environment for me to ask questions and discuss big decisions,” “I would not have had the opportunities or productivity I have had without my mentor.”
CONCLUSIONS
We successfully developed and incorporated an effective mentorship program for our PCCM fellows after identifying and addressing barriers. It is now an established and integral part of our PCCM fellowship program.
REFERENCES
1. Farag E, Abd-Elsayed AA, Mascha EJ, O’Hara JF. Assessment of an Anesthesiology Academic Department Mentorship Program. The Ochsner Journal 2012. 12:373-378.
2. Sambunjak D, Straus SE, Marusie A. Mentoring in Academic Medicine: A Systematic Review. JAMA.2006;296:1103-1115.
3. Morrison LJ, Lorens E, et al. Impact of a formal mentoring program on academic promotion of Department of Medicine faculty: a comparative study. Med Teacher. 2014; Jul;36(7):608-14.
4. Berk RA, Berg J, Mortimer R, Walton-Moss B, Teo TP. Measuring the Effectiveness of Faculty Mentoring Relationships. Acad Med. 2005;80:66-71.
5. Kashiwagi DT, Varkey P, Cook D. Mentoring Programs for Physicians in Academic Medicine: A Systematic Review. Acad Med. 2013;88:01-09.
Table 1: Mentoring Program Characteristics
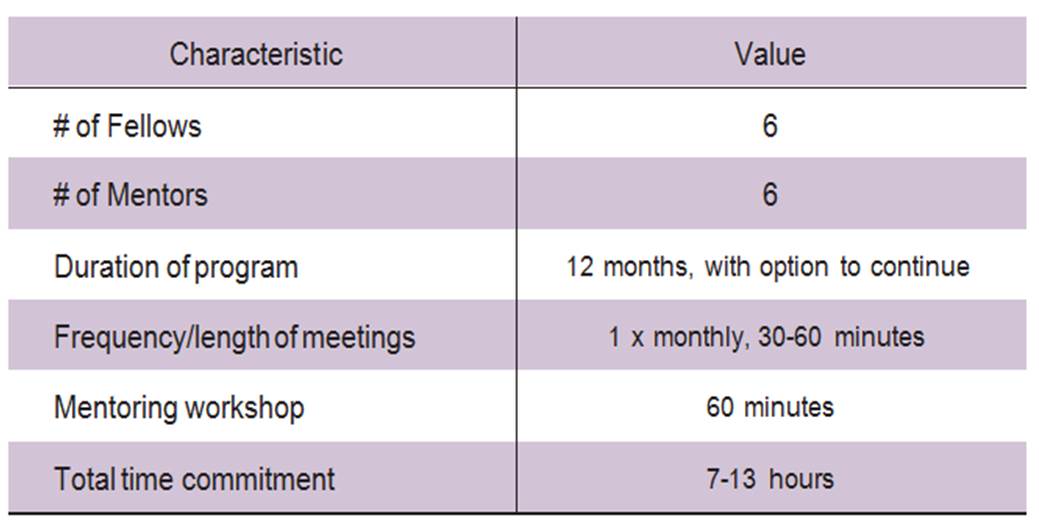
Table 2: Mentoring Evaluation Tool (Berk 2005)
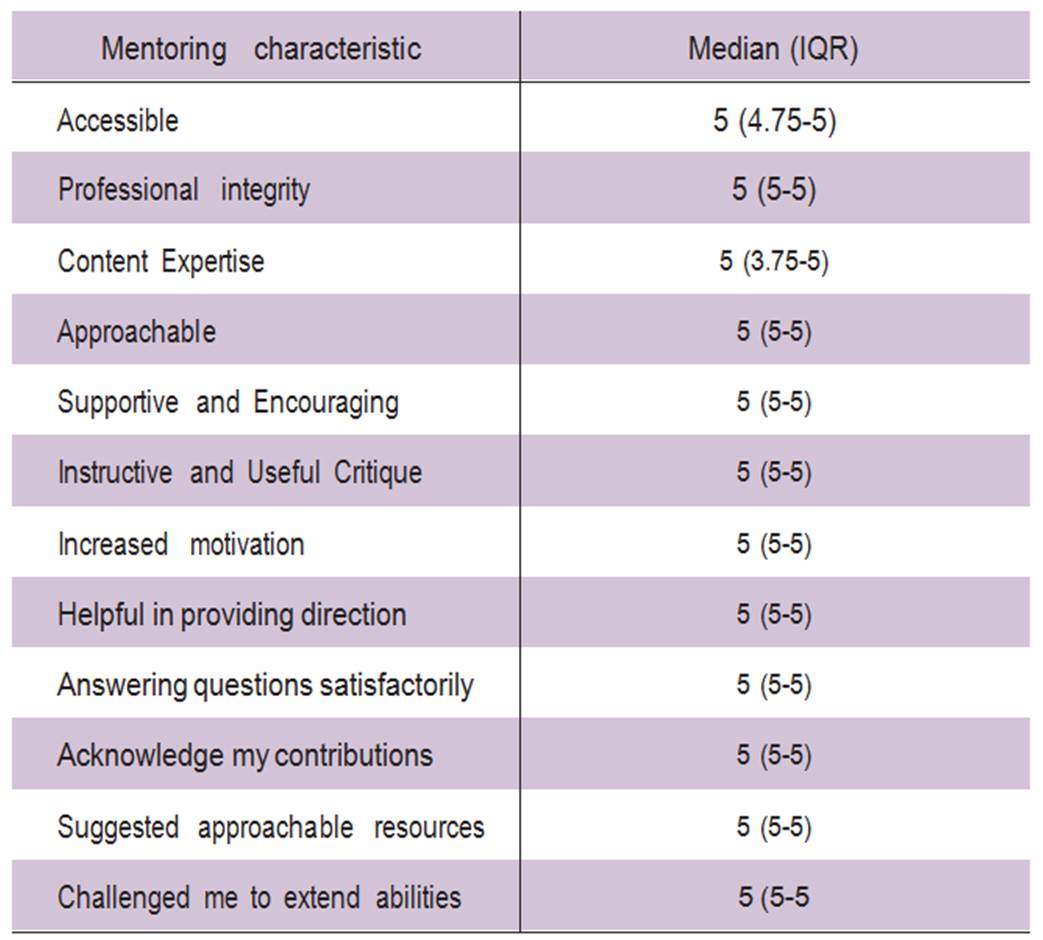
Chart 1: Fellow perceived Barriers to Mentorship (Pareto chart)




