Difficulty Swallowing
Sushilkumar Satish Gupta1* M.D., Nikhil Cordeiro2 M.B.B.S. Jessell Posada3 MS, CCC-SLP, Stephan Kamholz4 M.D.
1 Fellow, Department of Pulmonary and Critical Care Medicine, Maimonides Medical Center, Brooklyn, NY, USA.
2 Resident, Department of Internal Medicine, Maimonides Medical Center, Brooklyn, NY, USA.
3 Speech – language pathologist, Maimonides Medical Center, Brooklyn, NY, USA.
4 Chairman, Department of Medicine, Maimonides Medical Center, Brooklyn, NY, USA.
Case
A 67-year-old man presents with productive cough, shortness of breath and dysphagia of one-week duration. He has a history of laryngeal cancer treated with radiation and chemotherapy, and has residual left laryngeal nerve paralysis, as well as lung cancer which was treated by left upper lobectomy. He complains of regurgitation of solids and liquids through his mouth and nose when swallowing. A modified barium swallow study is performed and the findings are shown in Figure 1 and Video 1.
Question
What best describes the images you see in Figure 1 and Video 1?
- Schatzki’s ring
- Diffuse esophageal spasm
- Aspiration
- Zenker’s diverticulum
- Esophageal achalasia
Figure 1: Anterior-Posterior view of modified barium swallow study
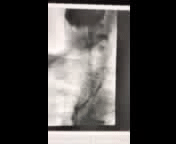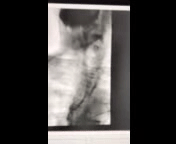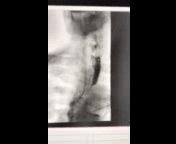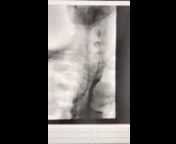
Video 1: Passage of contrast during modified barium swallow study
C. Aspiration
Discussion
The modified barium swallow study demonstrates silent aspiration of thin liquids, nectar thick liquids and puree. Mild tertiary contractions, slow bolus passage from the esophagus to the gastroesophageal junction, and contrast entering the right and left mainstem bronchi is observed. The patient has significant oral-pharyngeal dysphagia evidenced by decreased tongue base retraction, absent epiglottic inversion, incomplete laryngeal vestibule closure, and decreased upper esophageal sphincter opening, all likely attributable to late effects of radiation therapy.
Deglutition (or swallowing), facilitates the passage of food and fluids from the mouth, through the pharynx and into the esophagus, while closing the epiglottis.1 The four phases of swallowing include the oral preparatory, oral, pharyngeal, and esophageal phases. Swallowing begins with the voluntary oral phases, after which there is an involuntary reflex that involves rapid and accurate coordination between sensory input and motor function.2 This involves cranial nerves V, VII, IX, X and XII.
Patients with neurological deficits may have difficulty with either the oral phase or the pharyngeal phase or both. Impaired tongue movement while chewing or swallowing can cause food to fall into the pharynx and into the open airway before completion of the oral phase. A delayed pharyngeal swallowing reflex can cause food to fall into the airway. Decreased peristalsis in the pharynx can leave residue in the pharynx after swallowing, which can fall into or be inhaled into the airway. Dysfunction of the larynx or cricopharyngeus muscle can cause decreased airway protection during swallowing and hence lead to aspiration causing pneumonitis or aspiration pneumonia.
Long term complications of head and neck cancer treated with chemo-radiotherapy and surgery may include dysphagia and aspiration.2 Silent aspiration is the penetration of food below the level of the true vocal cords, without cough or any outward signs of difficulty.3 Patients with silent aspiration may not show any signs of aspiration during a clinical exam but it can be detected by the modified barium swallow study.2
The modified barium swallow study (MBSS), also known as video fluoroscopic swallow study (VFSS) uses barium and fluoroscopy to evaluate the physiologic and anatomic components involved in the swallowing process, as well as the integrity of airway protection.4,5 It is a non-invasive test with low dose radiation which helps determine which solid or liquid consistencies are suitable for the patient to ingest with the aim of preventing aspiration.1 Although the standard bedside swallow exam can identify patients who are at risk for or who have dysphagia, studies have shown that in comparison to a modified barium swallow study, the bedside exam is neither very sensitive nor specific in detecting aspiration.4 A combination of the modified barium swallow study and regular swallowing therapy can restore oral intake in more than 85% of dysphagic, neurologically impaired and surgically treated patients who have had head and neck cancer. In the absence of the MBSS, precise swallowing therapy cannot be planned and there would be an increase in time and money spent in attempting to evaluate and treat dysphagia.
(Choice A) Schatzki’s ring is a circumferential submucosal ring at the gastroesophageal junction. Most frequent presenting symptoms are progressive dysphagia to solid foods and commonly associated with improperly chewed meat, described as a sensation of food sticking in the chest. Barium swallow shows a concentric ring at the gastroesophageal junction.
(Choice B) Diffuse esophageal spasm is a motility disorder characterized by intermittent uncoordinated contractions of the esophagus. It commonly presents with dysphagia to solids and liquids, and atypical chest pain. Barium swallow shows a typical appearance of repetitive, non-peristaltic contractions that produce a "corkscrew" appearance.
(Choice D) Zenker’s diverticulum is a sac-like posterior outpouching of the mucosa and submucosal layers (false diverticulum), in the hypopharynx. It typically presents with a history of dysphagia followed by as sensation of food stuck in the throat and halitosis. Barium swallow delineates an outpouching lesion in the hypopharynx.
(Choice E) Esophageal achalasia is a motility disorder characterized absence of esophageal peristalsis and failure of relaxation of the lower esophageal sphincter. It typically presents with dysphagia for solids and liquids, regurgitation of undigested food, heart burn and chest discomfort. Barium swallow typically shows narrowing at the gastroesophageal junction in a "bird beak" configuration with proximal dilatation of the esophagus.
References
-
Peterson R. Radiologic Technology 2018: 89(3): 257-275.
-
Lee S-Y, Kim BH, Park YH. Analysis of dysphagia patterns using a modified barium swallowing test following treatment of head and neck cancer. Yonsei Medical Journal 2015; 56(5): 1221-6.
-
Teasell RW, McRae M, Heitzner J, et al. Frequency of videofluoroscopic modified barium swallow studies and pneumonia in stroke rehabilitation patients: a comparative study. Arch Phys Med Rehabil 1999; 80: 294–8.
-
Martin-Harris B, Logemann JA, McMahon S, et al. Clinical utility of the modified barium swallow. Dysphagia 2000; 15(3): 136–141.
-
Brady S, Donzelli J. The Modified barium swallow and the functional endoscopic evaluation of swallowing. Otolaryngologic Clinics of North America 2013; 46: 1009-1022.



