Echocardiography in Acute Multi-Organ Dysfunction
Andrew Badke, MD
Pulmonary and Critical Care Medicine Fellow
University of Utah School of Medicine
Presentation:
A 59 year-old female was discharged 10 days ago after receiving anticoagulation for a subsegmental pulmonary embolism that was provoked by surgical fixation of a tibial fracture. Over the subsequent weeks she began to develop increasing dyspnea on exertion, nonproductive cough, nausea, and generalized malaise. Prior to her hospitalization, she reported several months of mild dyspnea with exertion and intermittent lower extremity edema. On admission, she presented tachypneic, somnolent, and toxic appearing.
Physical exam:
BP: 97/57, HR 97, RR 24, Sa02 86% on room air.
Mild scleral icterus, jugular venous distension, bibasilar crackles, regular rhythm without murmurs; bilateral pitting edema to thighs, cool extremities.
Hospital Data:
BUN 68 mg/dL, Cr 1.43 mg/dL, ALT 3269 U/L, AST 4150 U/L, Bilirubin 3.6 mg/dL, INR: 8.2, WBC 13.8 k/µL
troponin 0.07 µg/L, BNP 2,493 pg/ml, lactate 11.2 mmol/L
EKG: Sinus rhythm with a normal axis and a previously documented left bundle branch block
Chest Radiograph: Bilateral pleural effusions, hilar congestion, cardiomegaly
Echocardiogram:
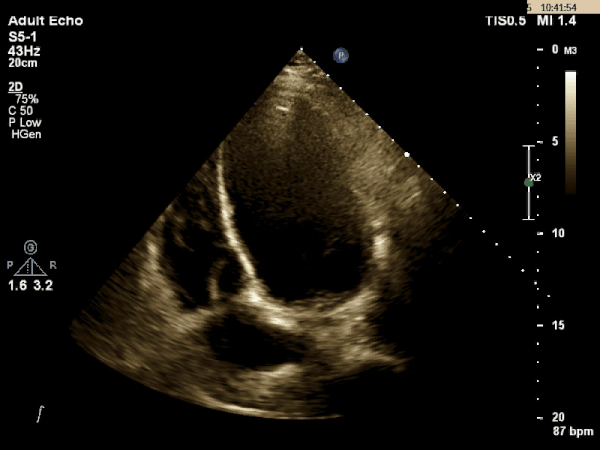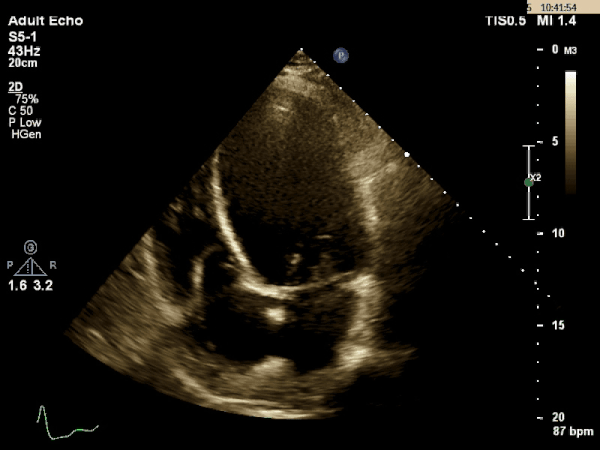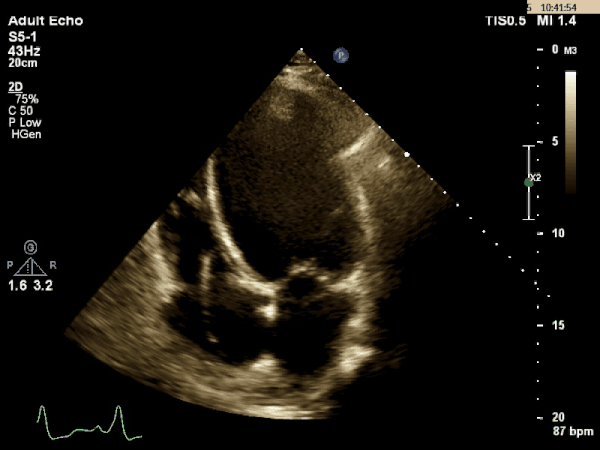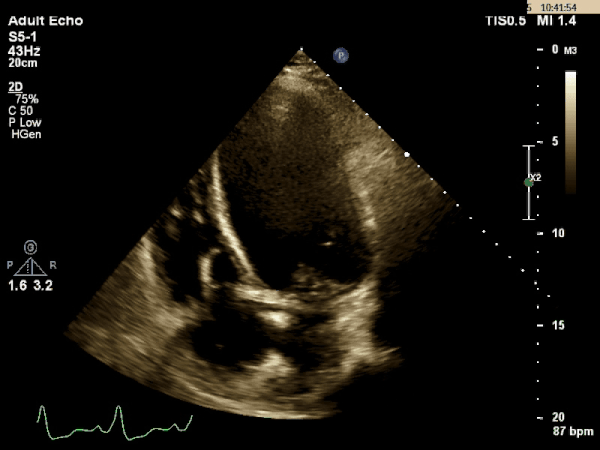
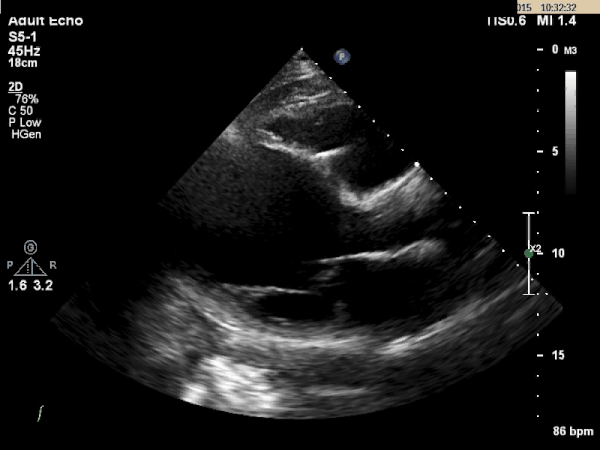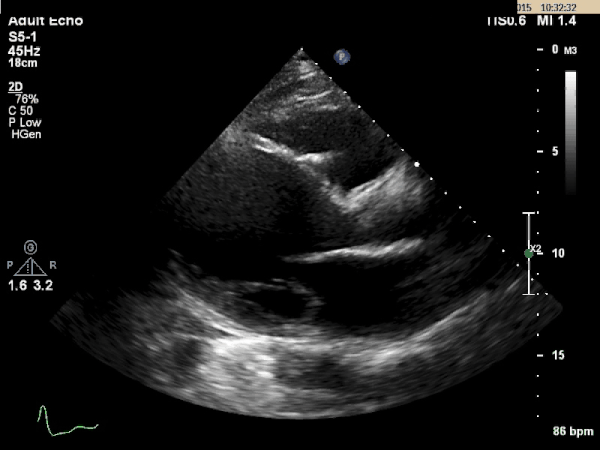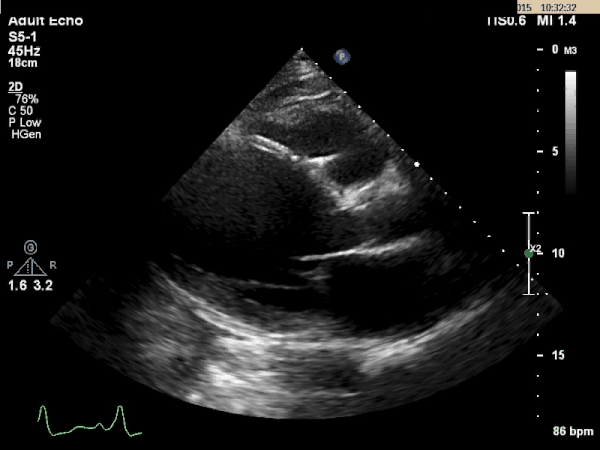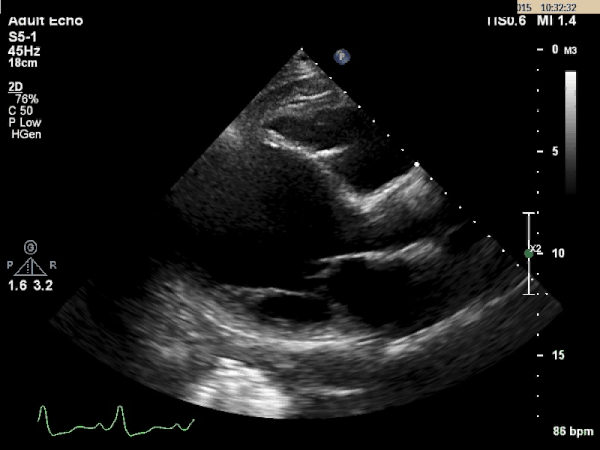
What is the most likely etiology behind this patient's multi-organ dysfunction?
Dilated Cardiomyopathy
The TTE images above shows a dilated left ventricle with severely reduced systolic function. The estimated ejection fraction is 9% and the LV internal diameter measures 6.36cm at end diastole and 6.25cm at end systole. These values are consistent with a dilated cardiomyopathy.
Dilated cardiomyopathy is a disorder characterized by a poorly functioning left ventricle in the absence of ischemic disease, and with normal loading conditions on the heart (no evidence of longstanding hypertension or valvular disease). Most patients with dilated cardiomyopathy will have asymptomatic cardiomegaly for weeks to months, but occasionally years can pass prior to diagnosis. Patients will typically present with indolent, progressive systolic heart failure symptoms. Rarely, patients can exhibit biventricular failure or even overt cardiogenic shock at the time of diagnosis.
Echocardiography is essential in diagnosing a dilated cardiomyopathy. The most widely applied criteria requires an ejection fraction of < 45% and/or a fractional shortening of <25%, as well as a left ventricular cavity dimension of >112% compared to predicted normal values.1 There are a number of different causes for dilated cardiomyopathy, some of which are reversible, while others are not (see list below). Diagnostic evaluation should begin with checking viral serologies, kidney, liver, and thyroid function tests, ESR, CK, calcium, phosphorus, and ferritin levels. If history indicates, then a toxicology screen, thiamine, and pyruvate levels can also be checked. Coronary angiography should be considered for patients with cardiovascular disease risk factors. Other more invasive tests such as skeletal muscle biopsy or endomyocardial biopsy may depend on the clinical history.
This patient’s multi organ dysfunction was secondary to biventricular failure with cardiogenic shock. She had no pre-existing cardiac disease or symptoms of heart failure. Her acute liver failure was likely a reflection of both hepatic congestion and inadequate perfusion. Once admitted, she had a pulmonary artery catheter placed, and received diuretics and dobutamine. With this, she was able to diurese multiple liters of fluid and her lactate subsequently normalized. Over the following days her liver chemistry and creatinine normalized as well. An extensive laboratory evaluation for work-up of her cardiomyopathy was negative and her angiogram was without evidence of coronary disease. Ultimately, the etiology of her dilated cardiomyopathy remains idiopathic. She currently is doing well on standard heart failure therapies.
Causes of Dilated Cardiomyopathy2
- Idiopathic
- Genetic:
- X-linked, mitochondrial, hemochromatosis, and familial syndromes
- Nutritional deficiencies*:
- thiamine, selenium, and carnitine deficiency
- Electrolyte abnormalities*:
- hypophosphatemia and hypocalcemia.
- Endocrinopathies*:
- thyroid disorder, cushings disease, pheochromocytoma
- Toxins:
- ethanol*, chemotherapeutic agents (doxyrubicin/cyclophosphamide), lead*, cocaine*, or mercury*.
- Infectious myocarditis:
- viral (cocksackie, CMV*, HIV, enterovirus), rickettsial, or parasitic (toxoplasmosis*, trichinosis, or Chagas’ disease)
- Inflammatory
- Collagen vascular diseases (scleroderma, lupus, dermatomyositis)
- Miscellaneous*
- peripartum, sarcoidosis, tachyarrhythmia induced, stress cardiomyopathy
* potentially reversible, either spontaneously or with treatment.
- Elliott P. Diagnosis and Management of Dilated Cardiomyopathy. Heart. 2000; 84 (1).
- Dec GW, Fuster VF. Medical Progress: Idiopathic Dilated Cardiomyopathy. NEJM. 1994; 331



