Contributed by Michael A. Passero, Jr, MD and Patrick Strollo, MD
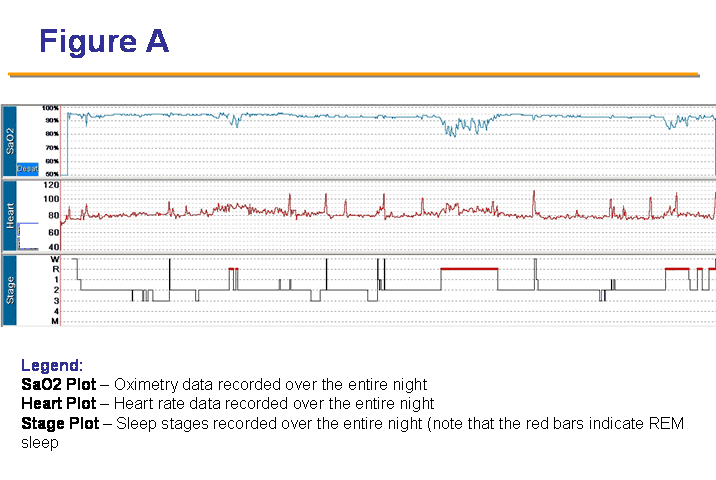
Figure A is the hypnogram from a diagnostic polysomnogram performed on a 40 year old, non-smoking, female. She complained of dyspnea, sleep disturbance and generalized muscle weakness. She denied snoring or observed apnea. Her weight was normal (body mass index [BMI] 22).
Questions:
- What is the key finding on the hypnogram?
- What would be the most likely diagnosis, given this history?
Question #1: REM related desaturation
REM related desaturation can be observed in restrictive disease limiting lung expansion due to alterations in the lung parenchyma (e.g. idiopathic pulmonary fibrosis), pleura (e.g. trapped lung), chest wall (e.g. obesity, kyphoscoliosis) or neuromuscular apparatus (e.g. primary neuromuscular disease, idiopathic disease of the diaphragm). It can also be seen in advanced obstructive lung disease. In obstructive sleep apnea (OSA) desaturation is usually worse in REM sleep however it is uncommon that desaturation is solely a REM related phenomenon. A characteristic desaturation pattern (i.e. "sawtoothing") is observed on the oximetry channel in most patients with OSA
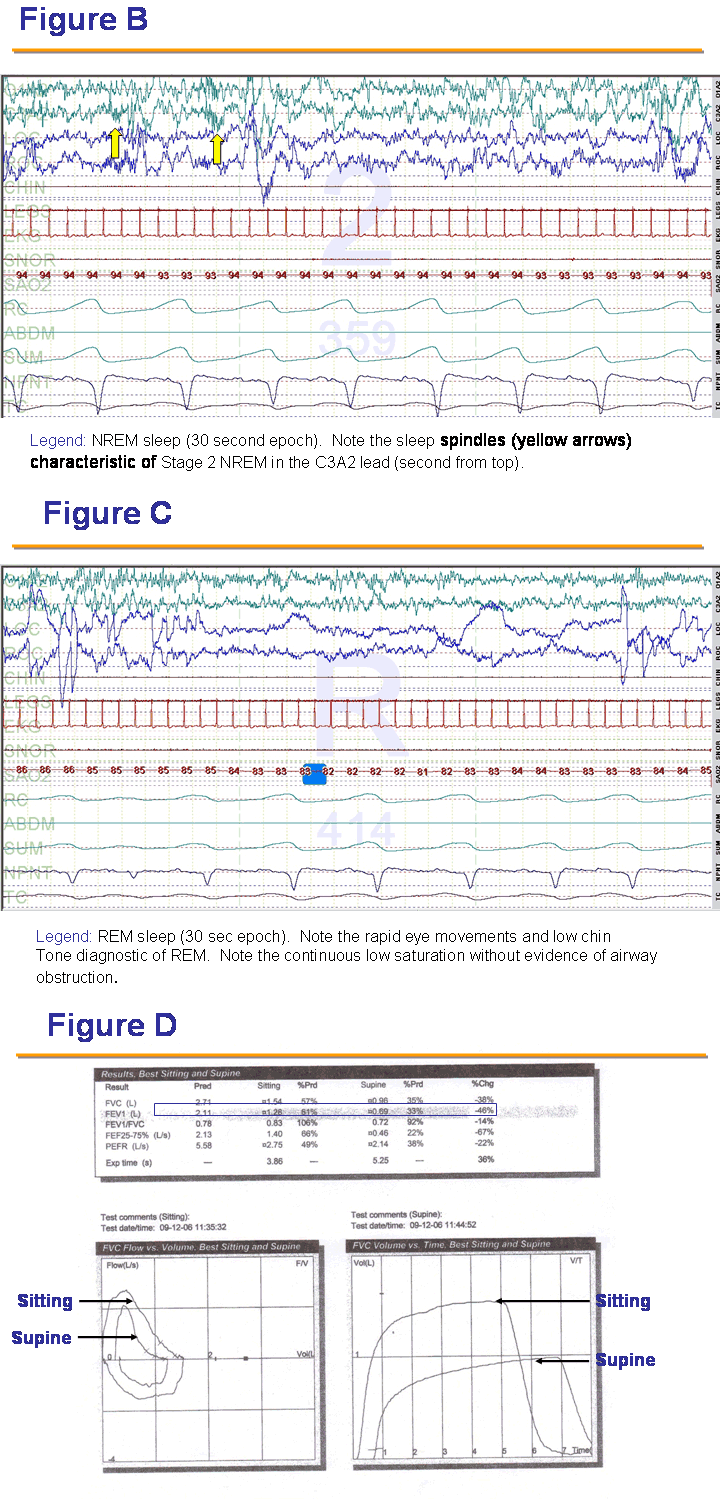
Figures B and C display two 30 second epochs from this study demonstrating REM specific desaturation on the oximetry channel.
Question # 2: Primary neuromuscular disease
The patient's history and BMI are most compatible with REM related desaturation due the neuromuscular apparatus. The ill defined muscle complaints suggest a primary neuromuscular disease as opposed to idiopathic bilateral diaphragmatic paralysis.
Subsequent testing confirmed the diagnosis of Acid Maltase Deficiency (Pompe's Disease), a glycogen storage disease that is associated diaphragmatic dysfunction, obstructive sleep apnea and respiratory failure. Enzyme replacement therapy is now available and may play a role in slowing progression of respiratory failure. Multicenter trials are currently ongoing.
Figure D displays her sitting and supine spirometry with accompanying flow-volume and volume-time loops. The significant decrease in the FEV1 and FVC are compatible with bilateral diaphragmatic weakness.
References:
- van der Beek NA, Hagemans MLC, van der Ploeg AT, Reuser AJJ, van Doorn PA. Pompe disease (glycogen storage disease type II): clinical features and enzyme replacement therapy. Acta Neurologica Belgica 2006;106(2):82-6.
- Hagemans MLC, Hop WJC, Van Doorn PA, Reuser AJJ, Van der Ploeg AT. Course of disability and respiratory function in untreated late-onset Pompe disease. Neurology 2006;66(4):581-3.
- Pellegrini N, Laforet P, Orlikowski D, et al. Respiratory insufficiency and limb muscle weakness in adults with Pompe's disease. European Respiratory Journal 2005;26(6):1024-31.
- Hagemans MLC, Winkel LPF, Van Doorn PA, et al. Clinical manifestation and natural course of late-onset Pompe's disease in 54 Dutch patients. Brain 2005;128(Pt 3):671-7.
- Winkel LPF, Van den Hout JMP, Kamphoven JHJ, et al. Enzyme replacement therapy in late-onset Pompe's disease: a three-year follow-up. Annals of Neurology 2004;55(4):495-502.
- Mellies U, Ragette R, Schwake C, Baethmann M, Voit T, Teschler H. Sleep-disordered breathing and respiratory failure in acid maltase deficiency. Neurology 2001;57(7):1290-5.