Mayo Clinic
Rochester, MN
Abstract Authors: Diana J. Kelm, MD; Joseph Skalski, MD; Kannan Ramar, MBBS, MD
Program Director: Kannan Ramar, MD
Type of Program: Pulmonary/Critical Care
BACKGROUND
Pulmonary and Critical Care Medicine (PCCM) fellows at our institution are responsible for the longitudinal care of their continuity clinic patient panel. These patients often generate paperwork or messages that require attention outside of regularly scheduled clinic time; such messages can be difficult to address if on a busy ICU rotation or on night shifts thus potentially resulting in a delay in a patient’s outpatient care. Additionally, our fellows teach medical students during their hectic half-day of continuity clinic, which can interrupt the fellows’ clinic flow and the teaching experience for medical students. To address these issues, we instituted an innovative pilot project of a new clinical role called the “Fellow of the Day (FOD)”.
METHODS
Our program has 3-4 fellows in the continuity clinic each half day. One fellow was assigned as the FOD and took responsibility to address patient care related messages or paperwork for any fellows away from their continuity clinic (i.e. in the ICU or on vacation) and teach the medical students. The FOD had a flexible schedule with fewer number of patients scheduled to help serve the above responsibilities. The FOD role was studied over a 4-month period. We collected data using an electronic survey (REDCap, Vanderbilt University, Nashville, TN) that was sent to medical students, PCCM fellows, and supervising staff. Survey responses were based on a Likert scale. For questions pertaining to teaching medical students and addressing priority messages while in the ICU, the scale ranged from 1-5 (never = 1; rarely = 2; every once in a while = 3; sometimes = 4; almost always = 5). The scale ranged from 1-5 (never = 1; once a week = 2; several times a week = 3; daily = 4; N/A = 5) for questions on how often fellows managed patient care related messages or paperwork while in the ICU or on their day off. Those that choose N/A for these questions were excluded in the analysis as they were not in the ICU during the time of this pilot study.
RESULTS
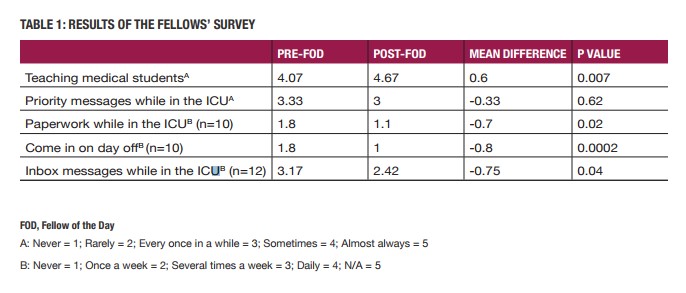
We surveyed multiple stakeholders about FOD including fellows, medical students rotating through clinic, and faculty. There were a total of 17 fellows in our PCCM fellowship program. Sixteen fellows (94% response rate) responded to the pre-FOD survey and 15 fellows (88% response rate) for the post-FOD survey. Table 1 highlights our results. Both medical students and fellows reported that FOD substantially improved the teaching experience: Nine (60%) fellows felt they were delayed in their continuity clinic when medical students were present before the FOD and only 1 (7%) felt delayed afterwards (p=0.002). After the FOD implementation, fellows were more likely to teach medical students (4.07 vs. 4.67, p=0.007). Medical students reported that they were more actively engaged in clinical patient care with the fellows (p=0.02) and enjoyed the teaching experience significantly post-FOD implementation (p=0.004). Fellows also felt that they spent less of their own time or time away from critically ill patients to focus on patient care related messages and paperwork after the FOD implementation. Thirteen fellows (87%) wanted to continue the FOD role at the end of the study period. The continuity clinic staff thought the FOD role was good for teaching, were satisfied.
DISCUSSION
The implementation of the FOD role was a huge success as it allowed PCCM fellows to have a more meaningful continuity clinic experience without disruption in clinic and ICU workflow, and improved the medical students’ teaching and clinical experience in the continuity clinic